Function of Liver
The liver regulates most chemical levels in the blood and excretes a product called bile. This helps carry away waste products from the liver. All the blood leaving the stomach and intestines passes through the liver. The liver processes this blood and breaks down, balances, and creates the nutrients and also metabolizes drugs into forms that are easier to use for the rest of the body or that are nontoxic. More than 500 vital functions have been identified with the liver. Some of the more well-known functions include the following
- Production of bile, which helps carry away waste and break down fats in the small intestine during digestion
- Production of certain proteins for blood plasma
- Production of cholesterol and special proteins to help carry fats through the body
- Conversion of excess glucose into glycogen for storage (glycogen can later be converted back to glucose for energy) and to balance and make glucose as needed
- Regulation of blood levels of amino acids, which form the building blocks of proteins
- Processing of hemoglobin for use of its iron content (the liver stores iron)
- Conversion of poisonous ammonia to urea (urea is an end product of protein metabolism and is excreted in the urine)
- Clearing the blood of drugs and other poisonous substances
- Regulating blood clotting
- Resisting infections by making immune factors and removing bacteria from the bloodstream
- Clearance of bilirubin, also from red blood cells. If there is an accumulation of bilirubin, the skin and eyes turn yellow.
Alcohol is filtered through the liver, but there is a limit to how much your liver can process. Having too much alcohol in your body makes it difficult for your liver to perform its necessary functions.
Drinking too much alcohol damages the liver, preventing or inhibiting it from doing its job.

How Alcohol Affects the Liver
It takes the body approximately an hour to process one alcoholic beverage. This time frame increases with each drink. The higher someone’s blood alcohol content, the longer it takes to process alcohol. The liver can only process a certain amount of alcohol at a time. When someone has too much to drink, the alcohol left unprocessed by the liver circulates through the bloodstream. The alcohol in the blood starts affecting the heart and brain, which is how people become intoxicated. Chronic alcohol abuse causes destruction of liver cells, which results in scarring of the liver (cirrhosis), alcoholic hepatitis and cellular mutation that may lead to liver cancer. These conditions usually progress from fatty liver to alcoholic hepatitis to cirrhosis, although heavy drinkers may develop alcoholic cirrhosis without first developing hepatitis.

TYPES OF ALCOHOL-INDUCED LIVER DAMAGE
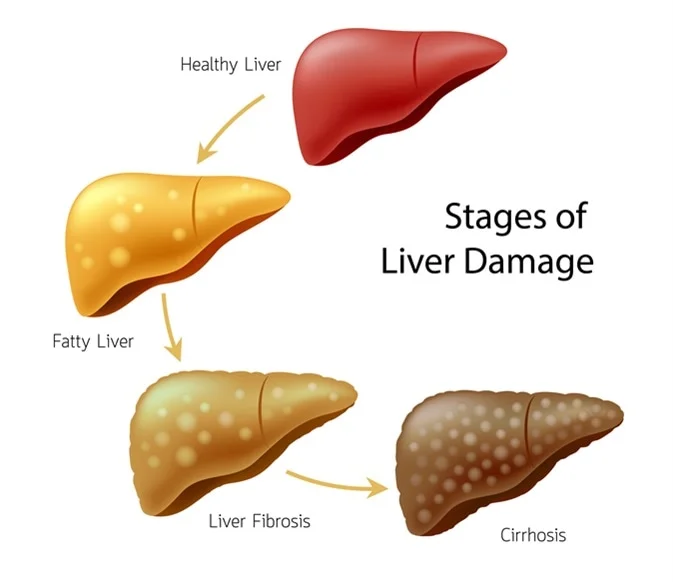
Alcohol-related liver damage can be divided into three categories :
(1)Fatty liver. Some degree of fat deposition in the liver occurs in almost all heavy drinkers. It also may occur transiently in non alcoholics after a single drinking session. Fatty liver is reversible and is not believed to lead to more serious damage.
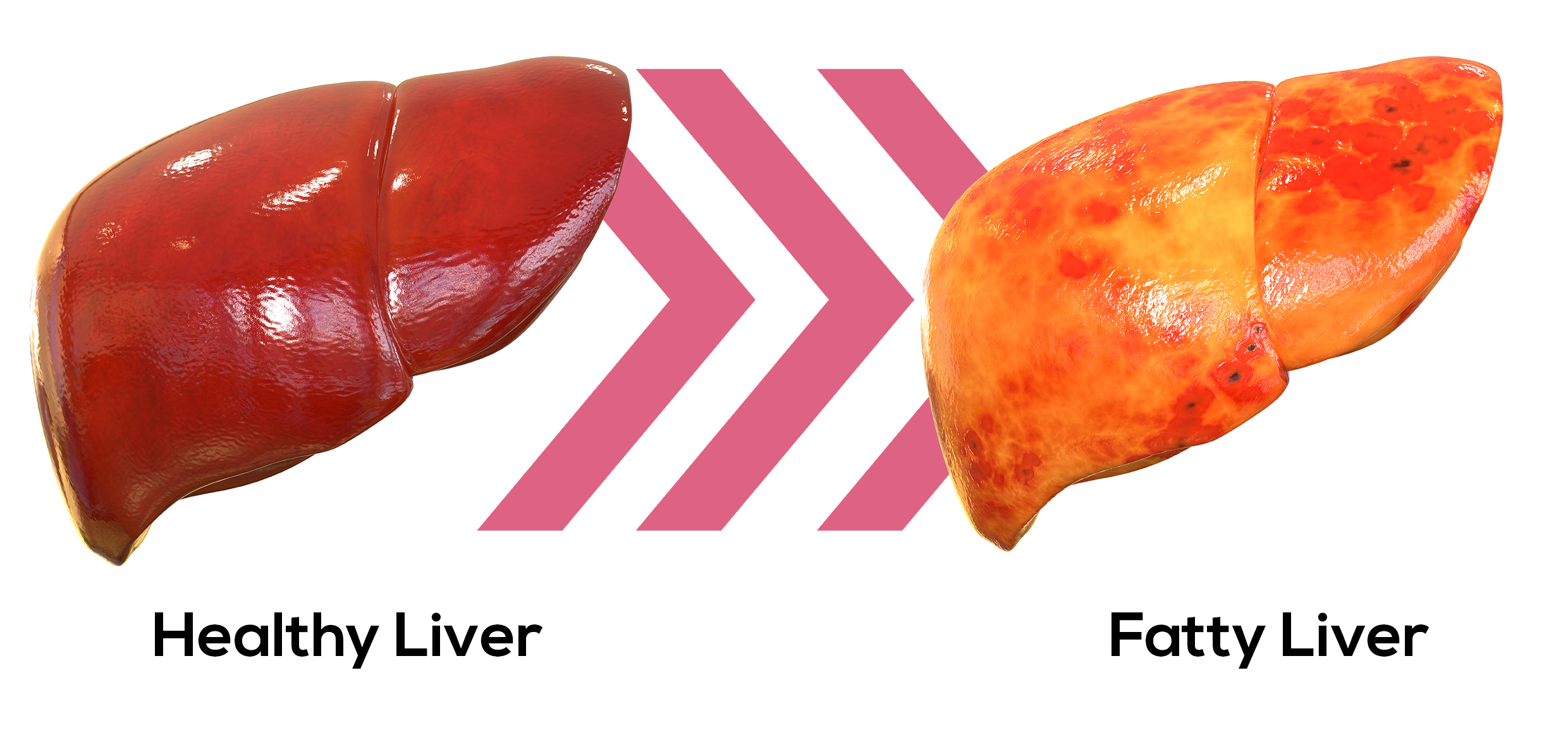
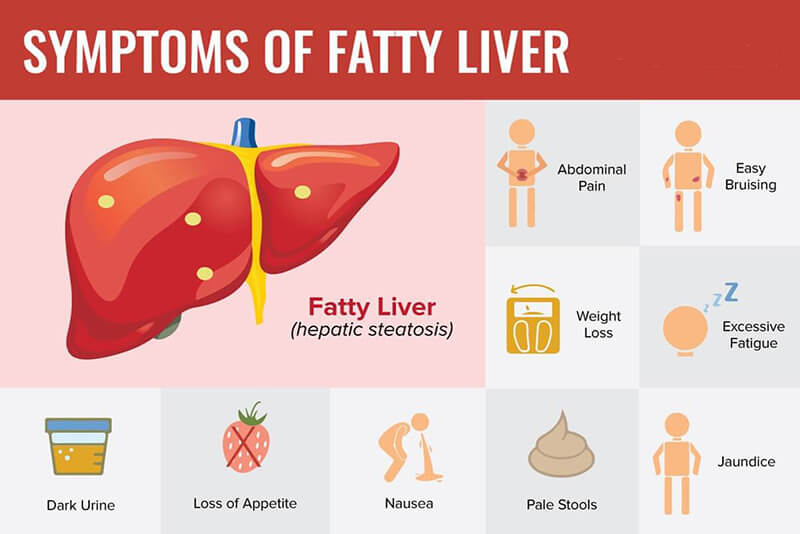
Symptoms
People with fatty liver disease often have no symptoms until the disease progresses to cirrhosis of the liver. If you do have symptoms, they may include:
- Abdominal pain or a feeling of fullness in the upper right side of the abdomen (belly).
- Nausea, loss of appetite or weight loss.
- Yellowish skin and whites of the eyes (jaundice).
- Swollen abdomen and legs (edema).
- Extreme tiredness or mental confusion.
- Weakness.
(2)Alcoholic hepatitis. This disorder is characterized by widespread inflammation and destruction (i.e., necrosis) of liver tissue. Scar tissue may begin to replace healthy liver tissue, a process called fibrosis. Symptoms of alcoholic hepatitis may include fever, jaundice,2 and abdominal pain. The condition can be fatal but may be reversible with abstinence. Alcoholic hepatitis occurs in up to 50 percent of heavy drinkers (National Institute on Alcohol Abuse and Alcoholism)
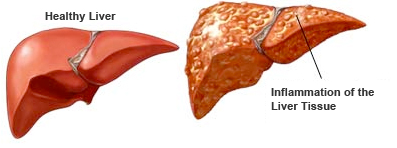
Symptoms
One of the most common signs of alcoholic hepatitis is jaundice, or yellowing of the skin and eyes.
Additional symptoms include:
- loss of appetite
- nausea
- vomiting
- stomach pain
- fever
- tiredness and weakness
- weight loss
Alcoholic hepatitis can be either mild or severe. It is possible to reverse the condition by ceasing to drink alcohol.
Severe alcoholic hepatitis can occur without warning, leading to life-threatening complications, such as liver failure.
(3)Alcoholic cirrhosis. This most advanced form of liver disease is diagnosed in 15 to 30 percent of heavy drinkers. Between 40 and 90 percent of the 26,000 annual deaths from cirrhosis are alcohol related . A cirrhotic liver is characterized by extensive fibrosis that stiffens blood vessels and distorts the internal structure of the liver. This structural damage results in severe functional impairment, which may lead secondarily to malfunction of other organs, such as the brain and kidneys. Although alcoholic cirrhosis is usually fatal because of complications (e.g., kidney failure and hypertension in the vein carrying blood to the liver [i.e., the portal vein]), it can stabilize with abstinence.
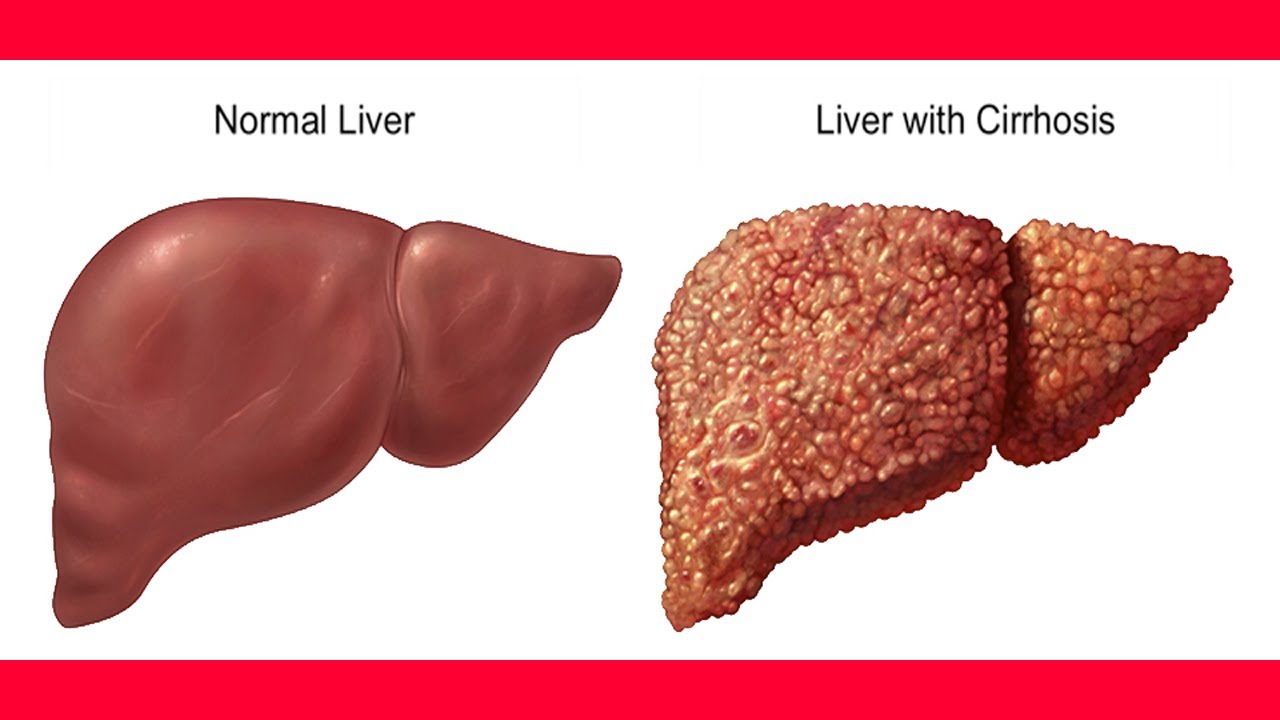
Symptoms of alcoholic liver cirrhosis include:
- Losing muscle tone (atrophy)
- Bruising easily
- Loss of appetite and weight loss
- Yellowing of the skin and eyes (jaundice)
- Fluid build-up and swelling of the legs (edema) and abdomen (ascites)
- Bleeding in your mouth (mouth bleeds) or vomiting blood
- Patchy red skin on the palms of your hands (erythema)
- Confusion, memory loss, poor concentration, and mental fog

Traditionally, these three conditions have been considered sequentially related, progressing from fatty liver to alcoholic hepatitis to cirrhosis. However, heavy drinkers may develop alcoholic cirrhosis without first developing hepatitis. Moreover, alcoholic hepatitis may have a sudden onset and a rapid course, causing death before cirrhosis can develop.
Treatment
The main treatment for liver disease is to stop consuming alcohol.
There is no cure for alcoholic liver disease, but treatment will aim to reduce or eliminate symptoms and stop the progression of the disease.
Scarring of the liver is permanent, but the liver can repair some of the damage. Treatment aims to restore as much normal function to the liver as possible.
Dietary changes: A doctor may also recommend dietary changes. Vitamin supplements or a focused diet plan may help to correct the balance of nutrients in the body if a person has malnourishment after regular alcohol use.
Medication: Doctors may prescribe medicines including corticosteroids and pentoxifylline to help reduce liver inflammation.
Liver transplant: In severe cases, a liver transplant may be the only chance for survival. However, the process of finding a donor can be long and complicated.
